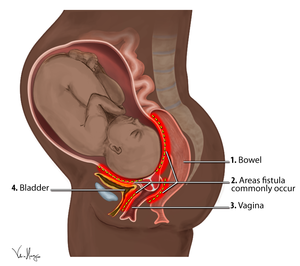
An obstetric fistula is an abnormal hole that forms between a woman’s vagina and her bladder or rectum. The opening forms after prolonged obstructed labour in cases where a woman in labour does not get medical attention quickly. According to the Fistula Foundation, fistula causes the woman to suffer urine and faecal incontinence. This causes affected women to be ostracized in many communities. The stigma thereof makes it harder for them to get help, yet obstetric fistula is a treatable condition. In this post, we share more details about:
- What causes an obstetric fistula
- Symptoms
- Complications arising from untreated obstetric fistula
- Treatment options
What causes obstetric fistula?
Prolonged obstructed labour
As mentioned above, an obstetric fistula develops as a result of prolonged obstructed labour. During labour, the woman’s body undergoes contractions in preparation for birth. As labour progresses, the baby’s head exerts pressure against the mother’s pelvic area. The delicate tissues found between the pelvic bone and the baby’s head are squeezed, thus cutting off blood supply. This may happen for two reasons:
- The woman has a small pelvis
- The baby is not well positioned, making it hard for them to descend through the birth canal
Following the lack of fresh blood supply, the soft tissues die, and this creates an opening – the obstetric fistula. This opening may form between the vagina and the bladder or rectum. This is what results in incontinence for patients with obstetric fistula. Incontinence is defined as the loss of voluntary control of urination or passing stool, thus leading to the leaking of urine and faecal matter.
Inaccessibility of Caesarean Section (CS) Services
Prolonged labour, particularly during the active stage of birth, places women at risk of complications, including obstetric fistula. To prevent these complications, doctors will often carry out an emergency CS. It is worth noting that in many cases, the benefits of a CS far outweigh the life-threatening birth complications that may follow.
In cases where women who need it do not get a C-Section in good time, there is a chance that one could develop an obstetric fistula. It is also important to mention that low quality CS may predispose a woman to fistula. The lack of important medical supplies and qualified doctors to assess the CS operation may also contribute to the fistula.
What are the symptoms of an obstetric fistula?
The most common symptom of obstetric fistula is urinary and/or faecal incontinence. This is a symptom that is characterised by the leaking of urine and/or stool through the vagina. In some cases, affected women may also pass gas or pus from the vaginal opening. This causes embarrassment and results in stigma and isolation for women with fistula.
Other symptoms associated with obstetric fistula include:
- Foul-smelling vaginal discharge
- Pain in the vaginal area
- Persistent UTIs (Urinary Tract Infections)
- Pain during sexual intercourse.
- Some women will also experience pain in the vagina and the perineum (this is the area between the vagina and the anus)
Complications that arise from untreated obstetric fistula
Women with fistula usually experience stigma, and are often isolated from their communities. As such, it is often difficult to get proper diagnosis and treatment for those living with the condition. This only serves to compound the complications that arise from an obstetric fistula.
Social impact of obstetric fistulas
Research shows that obstetric fistula affects women, both socially and psychologically. According to a report by the International Continence Society (ICS), the continuous leaking of urine and/or faeces causes affected women to produce an unpleasant smell. Consequently, these women face discrimination and social isolation. It is not uncommon to find women who have been rejected by their families and communities.
Physical and emotional abuse
In many African communities, a woman’s primary role is considered to be wife and a mother. One of the symptoms of an obstetric fistula is pain during sexual intercourse. As a result, many women are not able to have sex owing to the damage in the vaginal area. This, coupled with the leakage of urine and faeces often strains many relationships. It is not unusual to hear of divorce cases after a woman gets fistula. In addition, some women undergo physical and emotional abuse from their husbands, and this only adds to the distress.
Maternal Mental illness
An obstetric fistula significantly increases the chances that an affected woman will suffer a maternal mental illness. Of all maternal complications, an obstetric fistula is deemed to be one of the most damaging. The symptoms of the condition affect the quality of lives that the women lead, so much so that they are sometimes referred to as ‘dead women walking’.
Research shows that women with an obstetric fistula are at an increased risk of Postpartum Depression, Postpartum PTSD (Posttraumatic Stress Disorder) and other maternal mental illnesses.
Treatment of obstetric fistula
Diagnosis of an obstetric fistula includes a physical examination and, depending on the woman’s needs, tests to establish the location of the fistula. Once a diagnosis is made, effective treatment begins. The treatment of an obstetric fistula depends on a few factors, including the cause, size and location of the fistula.
Aim of treatment for obstetric fistula patients
Treatment of obstetric fistula provided for affected women seeks to improve the quality of life for affected women by:
- Ensuring the closure of the hole through surgical intervention
- Regaining urinary and faecal continence
- Restoring normal sexual life
- Helping make sure that the affected woman is able to deliver safely in future pregnancies
- Assisting the woman reintegrate in her society
Treatment options available for obstetric fistula
The successful treatment of obstetric fistula significantly improves the quality of life that the woman leads. Surgical intervention is an effective treatment option. Just as the name suggests, this process involves the closure of the fistula surgically. This procedure is carried out by experienced fistula surgeons. Sometimes, this poses a challenge as Kenya has few local skilled surgeons, too few fistula centres and sometimes, lack essential medical supplies for successful surgery.
In addition to surgical treatment, good hygiene and home remedies also plays a key role in the process of recovery. This includes drying the genital area thoroughly after passage of discharge and/or stool, the use of cotton underwear and loose clothing as well as products such as disposable underwear and adult diapers.
Check out the Fistula Foundation in Kenya for resources on where one can get treatment.
Works Cited
Ahmed, S., Genadry, R., Stanton, C., & Lalonde, A. (2007). Dead women walking: neglected millions with obstetric fistula. International Journal of Gynaecoloical Obstetrics, 99.
American Pregnancy Association. (2017, 03 24). Labour and Birth. Retrieved 04 03, 2019, from American Pregnancy Association: https://americanpregnancy.org/labor-and-birth/prolonged-labor-failure-progress/
Fistula Foundation. (2019). What is Fistula? Retrieved 04 03, 2019, from Fistula Foundation: https://www.fistulafoundation.org/what-is-fistula/fast-facts-faq/
International Continence Society. (2019). Obstetric Fistula: An Introduction . Retrieved 04 10, 2019, from International Continence Society: https://www.ics.org/committees/developingworld/publicawareness/obstetricfistulaanintroduction